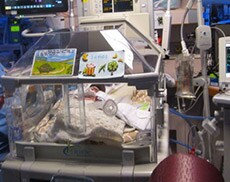
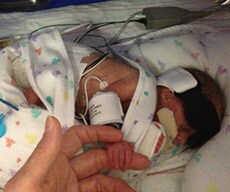
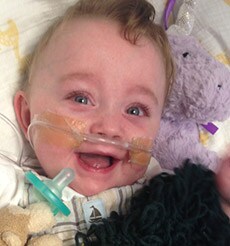
James was so fragile that the slightest movement, touch or sound sparked breathing problems that set off a chorus of beeps, dings, pings and rings from what seemed to be countless devices — a ventilator, chest leads, a pulse oximeter, blood pressure cuff and feeding pump. During the touch-and-go first few weeks, my husband and I constantly stared at the monitor showing his oxygen saturation, heart rate and respiratory rates, which weren’t stabilizing despite his being on 85% oxygen. We quickly learned which numbers set off which alarms and flashing lights, and which signaled that James was about to face another make-or-break moment.
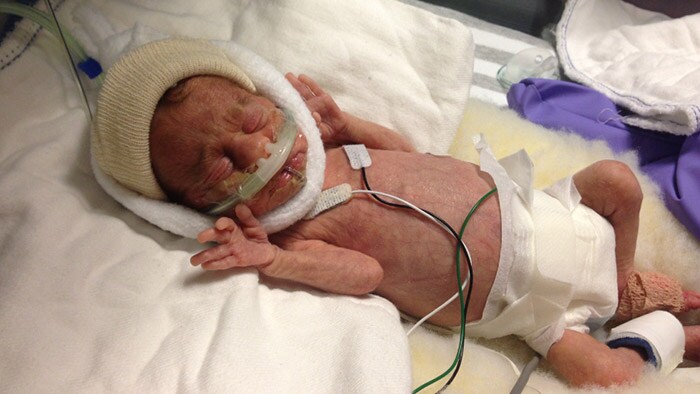
Strict parameters, unpredictable behavior
Sometimes when he dipped below set parameters, he would self-correct and begin to breathe again without intervention after about 30 seconds of “mellow yellow” alarming — the mild yellow flashing light and softer ding. Because it happened so often, the alarm was often silenced immediately and only drew attention when it kicked into the shrill red mode. At the same time, James started setting off false alarms. His micro-preemie skin was so thin that it needed to be moisturized regularly or it would actually tear. But the moisturizer caused his leads to slide off, which triggered a bad signal read and set off another alarm. On top of that, the sweat from his foot made it hard to keep the probe in place; if it wasn’t changed often, his pulse oximeter wouldn’t pick up accurately. It seemed that whenever his nurse turned away from his incubator to care for another baby, she couldn’t get more than a couple of meters away before James’ alarm sounded, insisting that she turn around. My husband and I joked that James was toying with them by holding his breath to purposefully sound an alarm — a sure sign of his prankish sense of humor. If James’ alarm went off for too long and his nurse wasn’t nearby, another nurse would usually look over and, more often than not, hit the silence button and see if he self-corrected. Even when the “mellow yellow” warning alarms turned into shrill emergency sounds — which happened every few minutes — it was often either a false alarm or his breathing would pick up. Except for the one time.
James’ Ping-Pong breathing—and the resulting near-constant alarming — didn’t improve over his first few weeks, or even months. His nurses responded quickly, and if repositioning him and turning up his oxygen didn’t work, they saved him with suctioning, a bag valve mask or by calling the crash cart team.
Other pages you might find interesting
5 key facts about alarm fatigue
Maintain effective protocols for ECG electrodes

A path forward: approaches for making effective change
An insider’s view of alarm overload
The perfect storm
But there wasn’t a nurse (or doctor) anywhere in sight. James’ oxygen saturation continued to plunge as his alarm flashed red, red, red. We pushed the emergency call button but nobody came. As our son started to turn blue before our eyes, my husband and I tore through the NICU to flag someone down. Not seeing anyone, I ran out to the receptionist so she could call for help. A nurse appeared and called for a crash cart. When the crash cart came, it came agonizingly slowly and by then, James was grey-blue and motionless. It took several more excruciating minutes to revive him.
What happened that day — when James was about 4 months old, still on high oxygen support and frequently yo-yoing — seems like a textbook case study in alarm fatigue, compounded by a confluence of other factors. It was around shift change and it was a holiday weekend, which meant a double-whammy of far fewer staff, and none of his usual nurses working. When the alarm went off signaling James was dipping, my husband and I watched his numbers fall — slowly at first, then precipitously — as we looked around for a nurse to respond.
Alarm fatigue and parent-nurse relationships
Even if heart-stopping close calls don’t happen, I think alarm fatigue can still negatively impact family members’ relationships with the healthcare team and cause them to lose faith in the hospital as a whole. Nurses know better than anyone that 99 out of 100 alarms may not require immediate attention. But what they might not know is how parents can interpret delayed reactions to alarms as complacency and unreliable alarms as indicative of untrustworthy equipment. For example, as a mother, I knew that a cumulative lack of oxygen could affect my baby’s nascent brain development, so every desaturation ignited deep reactions of helplessness and fear. Sometimes I felt that nurses silenced alarms as a reflex, and I noticed that every nurse had vastly different reaction times and levels of concern when it came to his alarming. Some nurses set his parameters differently, being personally comfortable with a wider margin. And a few even gave us permission to push the silence button ourselves if we determined it to be a bad read. While it was nice to be able to quiet the squalling alarms on our own without waiting for a nurse, having that responsibility — under a nudge-nudge, wink-wink jurisdiction — didn’t instill confidence that there were consistent policies in place to keep James safe. But I stifled my frustration. How could I expect busy nurses to stop what they were doing and constantly come over? I didn’t want to be a nuisance mum, compounding the annoyance of my baby’s nuisance alarm, and risk alienating the people who held his life in their hands.
Inevitably, that event changed the dynamic between our family and James’ care team, and a great amount of trust was lost.
...what other mothers experience when they hear their baby cry... My. Baby. Needs. Me."
Practically speaking though, why should it matter what parents feel? For me, the constant state of stress definitely affected my ability to produce and pump breast milk — which, of course, is immeasurably beneficial for preemies like James. And, less personally, studies show that parents’ stress during a NICU admission can influence the psychological and behavioral development of their baby, and that a trusted, positive relationship with their child's medical team can reduce these anxieties.
Impact on development
Even after James’ eye mask and earmuffs came off and he moved from an incubator to a crib, it was easy to see how much the noise affected him. This always increased his alarming and his need for more urgent care. The over-stimulation seemed to have lasting effects. It took more than a year before he could make eye contact, because he clearly found it too intense, and he cringed to the touch. After leaving the NICU (followed by eight months in a different hospital setting), James has made incredible strides. But even now at 4 ½, he still jumps out of his skin at unexpected noises. Is there a link between vacuums or blenders sending him into hysterics with his overstimulating hospitalization? I don’t know. But I do know that noisy toddlers (and which ones aren’t?) terrify him, and I worry about the impact this has on his ability to make friends.
There is little that parents can do about the constant din of staff conversations, cries of other babies, colored flashing signals and alarms that keep their baby from truly resting and effectively healing.
James was so delicate that Kangaroo Care couldn’t happen for several months, partly because he would desaturate at the alarm sounds. This was as frustrating as it was heartbreaking, as I knew that skin-to-skin contact has been shown to stabilize babies’ heart rates and improve their breathing; not to mention the bonding benefits.
My husband and I are both guilty of inadvertently tuning out his alarm, and over the years we have stopped immediately leaping to his side as soon as it goes off. I know that most of his alarms are false and believe I have a firm sense of his overall health, which dictates my responsiveness. Nowadays, part of “alarm management” is trying to stop James from pushing the silence button himself to stop the beeping — or turning the power off completely. “Making mischief,” indeed. That’s all to say that I truly understand how alarm fatigue happens. And despite the frustrations we endured and what I believe are long-term effects on my son’s development, I am fundamentally grateful for the care he received. I know that nurses suffer from the strains of their working environment every day. And I do believe that, if they could, they would respond to every alarm every, time — so that the one out of 100 times a baby truly needs them, they would be there.
Share this story
Share this page within your network
Other pages you might find interesting

5 key facts about alarm fatigue

Maintain effective protocols for ECG electrodes

A path forward: approaches for making effective change
An insider’s view of alarm overload